What is Sleep Apnea?
Sleep apnea is a common sleep disorder that causes frequent pauses in breathing during sleep. Most people with sleep apnea experience symptoms such as loud snoring and daytime sleepiness. The two main types of sleep apnea are obstructive sleep apnea ( OSA ) and central sleep apnea ( CSA ).
Obstructive sleep apnea, a narrowing of the airway during sleep leads to breathing disorders. Central sleep apnea is a breathing disorder caused by a lack of communication between the brain and the muscles involved in breathing.
These breathing interruptions reduce sleep quality and, if left untreated, can lead to potentially serious health consequences. It’s important to talk to a doctor if you think you may be at risk for sleep apnea so you can get any necessary testing and treatment.
Sleep apnea is a type of sleep-related breathing disorder, a group of sleep disorders characterized by abnormal breathing patterns during sleep.
People with sleep apnea repeatedly have reductions or pauses in breathing for short periods while they sleep. Although these gaps cause the person to wake up periodically and reduce the quality of sleep, there is also the possibility that it will not be noticed.
There are several types of sleep apnea, categorized according to the cause of the breathing disorders.
Types of Sleep Apnea
Obstructive sleep apnea
Obstructive sleep apnea ( OSA ) occurs when the airway at the back of the throat narrows or becomes blocked during sleep, which can cause snoring as air is prevented from passing through normally. In response to the airway obstruction, a person usually wakes up, with considerable tension in the neck muscles and takes several deep breaths, often accompanied by sounds such as snorting, snoring, or choking.
Obstructive sleep apnea is the most common type of sleep apnea. It is estimated to affect 10% to 30% of adults in the United States, but in many cases it remains undiagnosed.
Central Sleep Apnea
Central sleep apnea ( CSA ) involves a disruption in communication between the brain and the muscles that control breathing. As a result, breathing may become “shallow” and have temporary pauses.
The prevalence of central sleep apnea is low compared to obstructive sleep apnea. It is estimated that less than 1% of people have CSA .
Symptoms of sleep apnea include the effects of abnormal breathing at night, as well as the effects of reduced sleep quality during the day.
Symptoms of Sleep Apnea
Symptoms of Obstructive Sleep Apnea
Common symptoms of obstructive sleep apnea include:
- Excessive daytime sleepiness.
- Loud snoring often punctuated by gasps or choking sounds.
- Headaches in the morning that may persist for several hours after waking up.
- Dry mouth _ the fresh breath _
- Restless sleep with periods of wakefulness during the night.
- Increased need to go to the toilet at night.
- Irritability or irritability.
- Reduced concentration.
Some symptoms of obstructive sleep apnea may not be immediately noticeable to the person with the condition. For example, abnormal breathing and snoring may only come to a person’s attention after being noticed by their bed partner.
Many of the symptoms of obstructive sleep apnea can also be caused by other health problems, so the condition cannot be diagnosed by symptoms alone.
Symptoms of Central Sleep Apnea
Symptoms most commonly associated with central sleep apnea include:
- Abnormal breathing rate, such as breathing that slows, speeds up, and stops during sleep.
- Excessive daytime sleepiness.
- Waking during the night.
- Sudden shortness of breath or chest pains at night.
- Difficulty concentrating .
- Morning headaches . _ _
As with obstructive sleep apnea, it is normal for people with central sleep apnea to ignore their irregular breathing during sleep unless a bed partner or guardian points it out to them.
The cause of breathing disorders differs between obstructive sleep apnea and central sleep apnea.
Causes of Sleep Apnea
Risk Factors for Obstructive Sleep Apnea
The main risk factors for obstructive sleep apnea are related to age, gender, body weight, and certain anatomical features of the head and neck.
- Age: The risk of developing obstructive sleep apnea increases with age until a person is in their 60s and 70s.
- Gender: Men are generally more likely to have obstructive sleep apnea, especially in the early stages of adulthood.
- Head and neck anatomy: Obstructive sleep apnea occurs more often in people who have certain anatomical features, such as a large tongue and a smaller lower jaw.
- Body weight: Multiple studies have found a correlation between a higher body mass index and an increased risk of developing obstructive sleep apnea.
Studies have identified associations between various other factors and an increased likelihood of developing obstructive sleep apnea (OSA), but further research is needed to clarify their effect on the development of OSA.
- Smoking: Some research has found a significantly higher risk of obstructive sleep apnea in people who smoke cigarettes compared to people who have quit or never smoked.
- Hormonal abnormalities: Hormonal conditions such as hypothyroidism or overproduction of growth hormone can increase the risk of AAH by causing tissue near the airway to swell or contributing to a higher body mass index.
- Sleeping position: Sleep apnea can develop or worsen when people sleep on their backs because of how this sleeping position affects the shape and position of the tissue around the airway.
- Family history of sleep apnea: There is some evidence that a family history of AAH may increase a person’s risk of obstructive sleep apnea, which may be related to anatomical features in the head and neck that are shared among family members.
- Nasal congestion: Difficulty breathing through the nose is more likely to cause AAH.
- Use of alcohol and certain medications: Alcohol and certain medications are associated with an increased risk of obstructive sleep apnea.
- Certain medical conditions: People with certain medical conditions, including several heart and lung conditions, may be more likely to develop AAH.
Risk Factors for Central Sleep Apnea
Central sleep apnea (CAO) most often occurs as a result of another medical problem, such as an infection or injury affecting the brainstem, heart or kidney failure, stroke, or excess production of growth hormone. Studies have identified some additional factors associated with an increased risk of central sleep apnea.
- Age: People who are over 65 have an increased risk of breathing disorders associated with central sleep apnea.
- Gender: Central sleep apnea is more common in men, which may be related to the levels of certain sex hormones.
- Use of certain medications: Chronic use of opioid medications and certain prescription drugs and narcotics can affect breathing and has been associated with a higher risk of CHD.
- Being at high altitude: High altitude is associated with CAD due to the reduced availability of oxygen in high altitude environments.
Sleep apnea must be diagnosed by a doctor or sleep specialist, and there are several steps in the diagnostic process.
Health History and Sleep Apnea Screening
Evaluation for sleep apnea usually begins with a review of a person’s symptoms and overall health, as well as a physical exam. This test is designed to detect signs of sleep apnea and identify risk factors that could contribute to the condition.
There are many symptom tests. 2 of the most common are:
- The Epworth Sleepiness Scale
- Berlin Questionnaire
Although special testing is required to confirm that someone has AAH, the presence of symptoms can influence the diagnosis and help determine the severity of the condition.
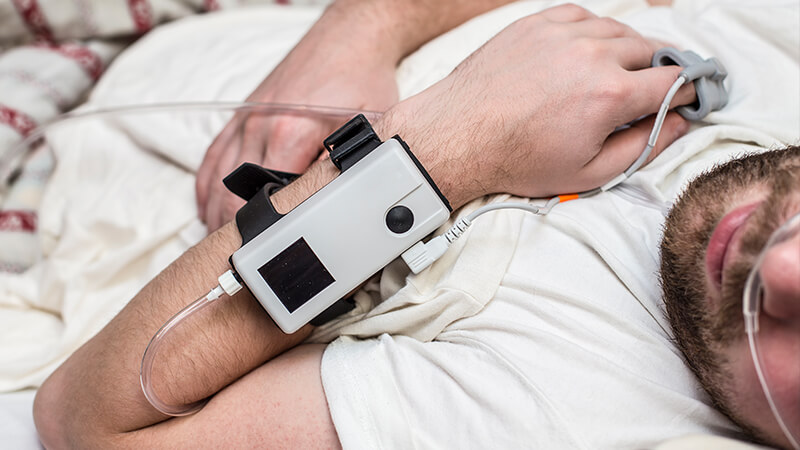
Diagnosis of Sleep Apnea
Sleep Study
A sleep study is necessary for the diagnosis of obstructive or central sleep apnea. The most reliable type of sleep study is called polysomnography ( Polysomnography ) , which is conducted during an overnight stay in a specialized sleep laboratory, in the hospital or at home.
During the sleep study, multiple sensors are used to monitor breathing, awakenings, oxygen level, muscle movement, sleep stages, and other aspects of sleep. A clinical sleep study can determine if breathing is abnormal and differentiate between obstructive and central sleep apnea. For AAH, polysomnography may include one or two visits to a sleep clinic or hospital.
A home sleep study for obstructive sleep apnea is an option for some patients who are thought to have more severe OSA. Taking a sleep apnea test at home may be more convenient, but the results should be interpreted by a healthcare professional. The home sleep test cannot diagnose central sleep apnea.
The goal of treatment for sleep apnea is to reduce breathing disorders and improve sleep. The treatment approach varies between obstructive sleep apnea and central sleep apnea.
Treatment of Sleep Apnea

Treatments for Obstructive Sleep Apnea
- Positive airway pressure ( PAP ) therapy
Positive airway pressure therapy ( PAP ) is a treatment offered to almost all people with obstructive sleep apnea. PAP therapy keeps the airway open with pressurized air pumped from a machine through a tube and a mask worn over the face.
PAP devices available only with a prescription. Their atmospheric pressure must be carefully calibrated, which takes place during a sleep study.
A common type of PAP therapy uses a continuous positive airway pressure ( CPAP ) device that sends a stream of air that is always set at the same pressure level. Other types of PAP devices , such as bi-level positive airway pressure ( BiPAP ) and auto-titration positive airway pressure ( APAP ), provide variability in the amount of air pressure.

- Sleep Apnea Splints
Sleep Apnea braces that hold the jaw or tongue in a specific position are a treatment option for people with specific anatomical features and less severe AAH. These mouth devices often do not improve breathing as much as PAP therapy , but studies in America have shown that they are used much more than PAP machines and are preferred by people who experience difficulty or discomfort when using PAP machines . In this way they can reduce or even eliminate snoring and reduce apneas to a very large extent.
- Surgery
There are many surgical methods to improve Sleep Apnea. Some of them are: Surgery to remove tissue in the neck, lengthen the jaw, and expand the airway may be a treatment option for patients who have tissue blocking their airway. Another type of surgical treatment requires implanting a device to stimulate a nerve that helps control breathing.
- Change of Habits
An additional component of treatment for obstructive sleep apnea includes lifestyle changes to help manage symptoms. They suggestions may include : _ _ _ _
- Decrease in body mass with weight loss.
- Regular exercise, which can reduce the symptoms of AAH. even without weight loss.
- Changing the sleeping position so that we do not sleep on our backs.
- Reduction of alcohol consumption . _ _
- Smoking reduction.
Treatments for Central Sleep Apnea
Treatment for central sleep apnea often focuses on treating the medical problem that is causing the abnormal breathing. If the sleep disturbances are mild, treatment for the underlying cause may be all that is required.
However, if symptoms of central sleep apnea are persistent or severe, additional treatment may be recommended to improve breathing while trying to resolve the underlying problem. This may include using PAP devices to promote steadier breathing during sleep. Other possible treatments include supplemental oxygen therapy or using drugs that can speed up a person’s breathing.
Effective treatment can generally prevent or resolve serious complications from sleep apnea, but if the condition is left untreated, it can have far-reaching effects on health and well-being.
Sleep apnea reduces the quality of sleep, and the effects of poor sleep are compounded by how sleep apnea affects oxygen levels in the body.
Effects of Sleep Apnea
Consequently, obstructive sleep apnea has been associated with a higher risk for a variety of health problems, including:
- Traffic accidents caused by youth . _
- Cardiovascular conditions such as high blood pressure, stroke, heart failure, heart disease and abnormal heartbeat.
- Metabolic disorders including type 2 diabetes.
- Pulmonary hypertension, which is high blood pressure in the arteries of the lungs that puts too much pressure on the heart.
- Thinking problems such as impaired memory and concentration
- Mood disorders, including irritability and a higher risk of depression.
- Non-alcoholic fatty liver disease, which is an increase in fat deposits in the liver that can contribute to severe liver damage.
- Complications related to anesthesia during surgery.
In central sleep apnea, the complications that may occur depend largely on the underlying medical problem that is causing the breathing disorder.
Although often associated with older adults, sleep apnea can occur in children. In young people, obstructive sleep apnea is much more common than central sleep apnea. It is estimated that 1% to 5% of children have obstructive sleep apnea.
Children with AAH may not experience excessive daytime sleepiness as seen in adults with sleep apnea. Instead, they may show symptoms during the day, such as hyperactivity , learning difficulties or behavioral problems.
As in adults, snoring is common for children with obstructive sleep apnea. However, children may have other symptoms at night, such as sweating, bedwetting or sleepwalking. Children with severe untreated AAS may also experience problems with their growth and development.
For many children, obstructive sleep apnea is caused by enlarged tonsils and adenoids in the throat, and surgery to remove these tissues may be a treatment option.
What should I do when I have Sleep Apnea?
Practical steps can help people living with sleep apnea cope with the condition and its potential health effects.
- Work closely with a doctor: It’s important to stay in touch with a primary care doctor or sleep specialist and report any ongoing symptoms, challenges with treatment, or other concerns that may require adjustments to your sleep apnea management plan.
- Take proper care of your therapy devices: Whether you’re using a PAP device or a Sleep Apnea splint, cleaning and maintenance can help you get the most out of your therapy and avoid unwanted side effects.
- Avoid high-risk activities: People with sleep apnea should be aware of the dangers of daytime sleepiness. Especially for people with untreated sleep apnea, activities such as driving or operating heavy machinery should be avoided when sleepy.
- Consider changing your sleeping position: Although they haven’t been rigorously studied, special products to avoid sleeping on your back may help some people reduce their obstructive sleep apnea symptoms.
- Minimize your alcohol consumption: Reducing your alcohol intake can be a component of your sleep apnea treatment plan. In people with untreated AAH, even drinking alcohol during the day can make breathing problems worse at night.
- Tell your new doctor about sleep apnea: People with sleep apnea should mention this condition to any new doctor, especially when you plan to start a new medication or have surgery.
At Galani Dentistry, our specially trained Doctors can advise you on the treatment of Sleep Apnea, and suggest solutions that will improve the quality of your sleep.




